Disclosure: this post contains affiliate links and if you purchase through my links, I will earn a small commission at no charge to you.
A little late to the party in sharing this as Caleb just turned 7 months old, but I’m glad I’m finally getting to write about his entrance into the world! When I found out I was pregnant, I had mixed emotions. I was definitely grateful, but at the same time had a lot of anxiety due to having a previous miscarriage and also being at my heaviest weight, ever. It did not feel like the best timing as I had been struggling to maintain a healthy weight and I had so many plans to detox and fix some of my own health issues before becoming pregnant, so I was plagued with guilt about how my weight might affect the baby. I don’t hear much about this compared to postpartum depression, but I struggled with depression early on in my pregnancy. Just sharing that in case you might be feeling similar things – you are not alone.
Once I made peace with the fact that I needed to do the best I could with where I was, healthwise, I tried to do everything possible to stay healthy and protect Caleb from harm, including things like wearing an EMF blocking belly protector when I was using my phone or computer. I also tried to avoid foods with folic acid and get plenty of folate and choline! As pregnancies go, mine was fairly uneventful and I didn’t have morning sickness or much pain until the very end, so I’m grateful for that. I credit regular chiropractic adjustments and massages for keeping me pain free and a prioritizing mineral balance, electrolyte hydration (thanks Earthley) and nutrient dense foods for avoiding nausea. I also highly recommend Ina May’s Guide to Childbirth as this gives so much valuable information on natural birth and POSITIVE birth stories, along with exercises like pelvic rocking that help keep the baby in an optimal position and prepare your body for labor.
I wanted to have a natural, unmedicated birth, and my heart was set on having a water birth as well because I feel most at peace when I’m around water and it seemed like it would help to relax me and ease the pain. I completed the needed online course to be eligible for water birth at Cone Hospital, but thought it was strange they only had 2 birthing tubs for a hospital that large. Apparently not many women opt to use the tubs – later on I realized why.
I started off seeing an OB-GYN for my prenatal care, but switched over to the midwives in the same practice as they were the only ones who were trained in water birth and I felt their birth philosophy aligned more closely with what I was hoping to achieve in my labor and delivery. I later learned that there are midwives and then there are MEDwives. It’s key to know the difference and interview them beforehand, but I digress 😉
I also took birthing and breastfeeding classes that were offered by our doula group and was glad to have them as a resource. All this to say, you can do everything you’re aware of to prepare for birth, but there will likely be so many things that are still out of your control, which is scary (and frustrating). As my doula helped me create a birth plan, she emphasized the importance of flexibility.
As it turns out, I’m so glad she prepared me for the different scenarios that could arise because one of them happened to me. As I mentioned, my pregnancy was uneventful, except for the fact that at each visit, my blood pressure was elevated. This can be a huge concern as it sometimes means you’re at risk for developing pre-eclampsia and/or HELLP Syndrome, but in my case I was tracking my BP daily at home and registering normal readings there, so I went back and forth with the midwives at each visit, letting them know my home readings were fine and that I had a history of “white coat syndrome” where blood pressure elevates in a medical setting due to anxiety.
They mostly accepted my home readings, but at my 30 week visit, they sent me to the hospital for monitoring because they felt it was too high. I stayed there about 2 hours until it dropped back to normal and I was able to go home that evening. They strongly suggested that I start on blood pressure medication, but I was not convinced it was an actual blood pressure issue as my home readings were still fine and I had no history of high blood pressure. I declined medication because I knew there could be side effects for the baby, and focused on following the Brewer Diet which is customized to help pregnant women with blood pressure issues. I learned that it is often a blood volume issue and that blood pressure issues in pregnancy are also directly linked to nitric oxide levels; this is definitely something I wish I had known so I could have addressed that. I know I’m sharing a lot of extra details here, but my hope is that my story can help someone else avoid the issues I had by focusing on these things early on.
I continued to have weekly prenatal visits up until my 37 week visit, where my blood pressure was high enough that they said I needed to return the next morning to have it checked again. Other than some swelling in my hands and ankles, I didn’t have any other signs of pre-eclampsia and my bloodwork all came back normal. I was trying to remain optimistic but asked Gabe to go with me to the visit the next morning because I was feeling nervous about what might happen.
My systolic readings the next morning were in the high 160’s and 170’s which they said put me at risk for a stroke and the midwife recommended induction that same evening for the safety of me and the baby. The good news was that I had reached 37 weeks which is technically considered “full term”, but everything in me was wanting to avoid induction because of how many negative stories I had heard about it and how it was almost impossible to avoid pain meds and/or epidurals and the “cascade of interventions” that often result after an induction.
I tried to remember that God’s hand was guiding us, even with an undesired and unexpected induction looming. We went home from the visit and agreed we’d return to the hospital at midnight to start the induction process. I hadn’t packed a hospital bag yet or finished most of the things I wanted to have ready at home, but Gabe was SUCH a blessing in packing things up and getting them ready, quickly tying up our loose ends as I was told I needed to be on bed rest until that evening. They told me to sleep as much as possible before I came in, but that didn’t happen because I was too nervous just running through everything in my mind!
We got to the hospital at midnight, marveled at the free valet parking (I was surprised to see plenty of other pregnant women there checking in at that time too – I guess midnight is popular for scheduled inductions?) and got situated in a room in the Cone Women’s Hospital in Greensboro. After we were in the room, they mandated that I get the first COVID test of my life which I wasn’t happy about (Gabe didn’t have to get one – lucky guy), and they put in a hep lock IV in my hand in case I needed medication in a hurry – that thing hurt so much especially when I bumped it on things!
I didn’t stay in the scratchy, oversized hospital gown for long – definitely changed into my own robe from home and felt much more comfortable that way. I also told the nurse I had no intention of wearing a mask during labor and no one had issues with that, so I’m thankful they weren’t sticklers in that situation.
After I was in the room for about an hour and all hooked up to their monitors, one of my midwives and her student came in to talk about the plan for induction. They asked to do a cervical check to see if was dilated at all and I was not, which wasn’t really a surprise considering I was only 37 weeks along. One thing no one prepared me for – cervical checks hurt – a LOT! Shortly after that, they gave me the first dose of Cytotec at 2:00 am (which serves to thin the cervix) in an oral tablet that dissolved in my cheek. I want to add that Cytotec is NOT an FDA approved medication and I definitely had concerns about taking it, but wasn’t aware of any other options available to start the process, so I begrudgingly agreed to it. I was adamant about not wanting any Pitocin as I had seen plenty of research about the dangers and side effects of that drug along with the fact that it often makes contractions so unbearable that you need an epidural.
They checked me again after 4 hours and I was only 1 cm dilated after some mild contractions. At this point they offered me some Ambien so I could try to sleep for a while. Normally I wouldn’t want any medication like that, but I gladly took it because I knew I would need sleep and rest to make it through labor and it definitely helped me fall asleep for a few hours.
I got the second dose of Cytotec and after 4 more hours, I was still at 1 cm so they gave me a third dose which got me to 2 cm. So discouraging to feel like I was barely making any progress. After the third dose, the next step we agreed on was them putting in a Foley balloon which they can gradually inflate (this is a more gentle method of dilation rather than using Pitocin) and that’s when contractions started to get intense and close together.
After having the Foley balloon in for 2-3 hours, I was still only at 4 cm and completely exhausted, so I was almost ready to ask for an epidural because of the pain and failure to make much progress. I also threw up 3 times during labor – nothing would stay down, which made it so hard to keep my strength up. It’s so key to be hydrated with electrolytes going into the birth process and to keep drinking throughout if you can keep it down! Thankfully I didn’t get to the point of needing IV fluids.
My doula got to the hospital around that point because I was struggling with so much pain and I was relieved to have her there for advice on how to manage the rest of the labor process. Gabe had been such a wonderful support up until that point and walked around the hospital halls with me for hours; walking was really the only thing that helped relieve any pain. He needed a break though as he barely had any sleep either, so it was good timing for the doula to arrive. She helped talk me through the pain and reasons why I wanted to stay unmedicated as I was saying that I think I needed an epidural. After talking with her, I decided I’d try to last a little longer without interventions. Other natural pain relief options I didn’t use: a comb for acupressure, TENS unit, and sterile water injections (can be used for relieving pain with back labor – thankful I didn’t experience that!)
Minutes later I felt an unnerving “pop” and the nurse thought it was the Foley balloon coming out (which would mean it had served its purpose) so she pulled it out only to find that my bag of waters had ruptured. It was a scary feeling as they didn’t want them to rupture just yet. They checked me after that, still at 4 cm but 80% effaced. I leaned hard on Gabe for the contractions that followed. No position felt good, massage and pressure did not help at all, and definitely hated the peanut ball they tried to get me to use! I think I got in the shower briefly but that didn’t feel good either. I was so overheated that even though they said I could use the birthing tub if I wanted it, I had no desire to get in it because it would be warm water and I was roasting! It’s funny how the things you have your heart set on change when you’re in the heat of the moment, ha!
Everything hurt so badly and it was difficult to breathe through each contraction – I definitely couldn’t talk. They thought about giving me more Cytotec but my contractions seemed strong enough on their own so they said my body was taking over (finally). When I was about 15 minutes away from asking for an epidural, I felt a strong urge to poop and went to toilet only to feel like I had to push, and I asked in a panic, “how do I stop it???” The nurse looked somewhat amused but also a little scared because she didn’t expect me to be fully dilated yet.
Another strong preference I had was to NOT give birth on my back, as I knew it wasn’t conducive to helping the baby out and often leads to tearing. I was hoping to kneel or stand and use the knees in calves out (KICO) position. Well, as it turned out I had stabbing knee pain that came out of nowhere in the few weeks leading up to labor and couldn’t even kneel for a few seconds without writhing in pain. That was disappointing to me that I couldn’t be in what I felt would be the best position for birth, but I didn’t have much time to dwell on it.
The doula and nurse then helped me into the bed to get ready to push and checked me to find I was fully dilated (hallelujah) but Amanda (our midwife) wasn’t there yet because I completed dilation more quickly than expected. When she got there she coached me on pushing only when each contraction hit and held a warm compress on me to prevent tearing, bless her! Pushing wasn’t fun but was nothing at all compared to the pain of contractions!! I probably pushed for about 15-20 minutes until he was delivered and they put him on my chest. He was born at 7:15 pm, so it ended up being about 17 hours from the time they started the induction process until he was born – incredibly grateful it didn’t go longer, as most people say first babies can mean labor lasting 24+ hours.
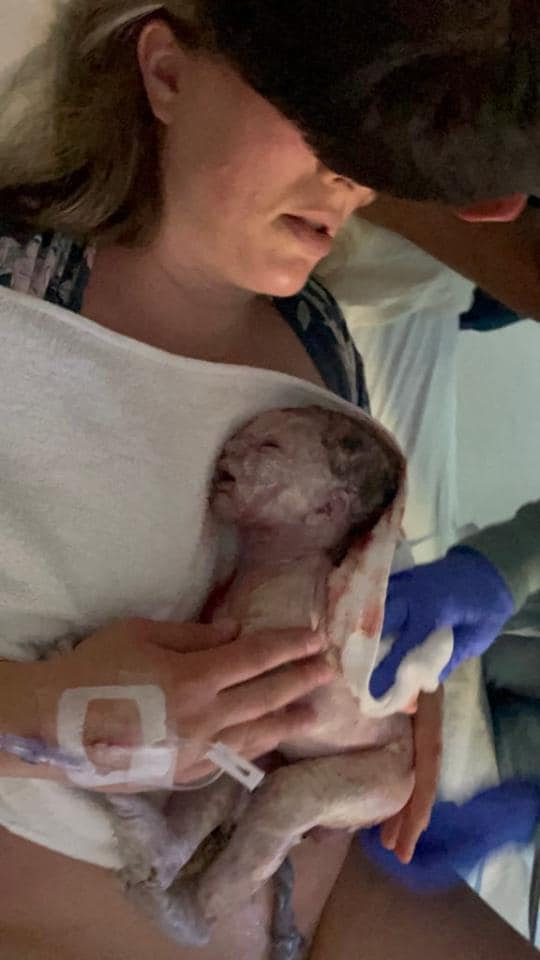
What a crazy feeling to see and hold my very own baby. The adrenaline was rushing and I felt such relief. I thought I would cry but didn’t. Gabe got to cut the cord once it stopped pulsing – I was so thankful the midwife was patient and didn’t rush that process. I next birthed the placenta within about 10 minutes then Amanda stitched up a minor first degree tear. I couldn’t stop shaking after Caleb was born due to hormones trying to regulate – it was wild. Gabe told me that Coldplay’s “A Sky Full of Stars” was the song playing while he was being delivered – how cool, as they’re one of my favorite bands. I may have stacked the birth playlist just a wee bit.
I was able to have skin to skin contact and breastfeed for a little while before they did all the standard tests on sweet Caleb. While they were doing that, our doula fed me a sandwich that was the most amazing meal of my life, because I was starving after not being able to eat during labor! Definitely took advantage of the snack room at the hospital – oh yes, that’s a thing! Italian Ice was my favorite from their selection.
After things settled and we got cleaned up, we got to go upstairs to the mom and baby room. We had to stay there 2 nights and it felt like nurses came in about every single hour throughout the day and night to do some kind of tests or give us paperwork; not much sleep happened, that’s for sure. I saw probably 5 different lactation consultants there and the nurses did fundal massages on me every 4 hours (this helps the uterus to contract and avoid excess bleeding). Those massages were the devil! One cool thing we only found out as we were about to leave the hospital was that Gabe’s cousin ended up having her baby 24 hours after Caleb and she was actually in the room right next to us!

All the nurses and hospital staff were excellent and Cone is an ideal place to give birth, in my opinion. I know hospitals get a bad rap sometimes, but they were all respectful of my sometimes unconventional requests and didn’t push things on us after we declined them once.
Whew! That was a lot of detail, but my hope in sharing all this is that it can give hope to other women who may end up in a similar situation with blood pressure or an induction. Also, I still have a ways to go to be at a healthy body composition, but by God’s grace, I’ve been able to lose the baby weight and have gone 15 pounds below my pre-pregnancy weight. It’s been a blessing to see how God has shown me that His timing is perfect and that He’s able to redeem any situation, even when it may at first seem bleak. Though at times I grieve not being able to experience labor starting on its own in a natural way, ultimately I’m just incredibly grateful for the blessing of baby Caleb and that he was born without any complications!
There is a lot of fear out there around unplanned induction, especially in the natural health community or those seeking natural birth, BUT it does not automatically mean that you’ll need pain medication or an epidural just because you’re being induced. I don’t consider myself to have that high of a pain tolerance, so I’d just encourage you to bring up questions about more gentle induction methods that your provider has available, so you’ll be informed of your options. They also offered nitrous oxide as a pain management option, but due to having the MTHFR genetic mutation, I wasn’t a good candidate for that (certain types of anesthesia can be unsafe for those with the mutation).
For anyone in my area (Greensboro/Kernersville) seeking a provider, I also want to say that Amanda Jones is my absolute favorite of all the midwives I saw at Wendover OB-GYN. She has a laid back demeanor that is calming, she listens so well, and she took extra steps to make sure I felt as empowered as possible in a situation where so many things were outside of my control. She even texted me a few days after his birth to check on me. That is truly going above and beyond and I so appreciate that she was the one that was on call for my labor (I know God orchestrated all of that).
I know many of you prayed for us during Caleb’s birth and I truly appreciate all of you! I can’t link to the doula I used since she’s on hiatus, but she was wonderful as well! If you have any questions about natural birth or doula options in the Triad, feel free to reach out or comment below.
Thanks for reading!
Emily


Thank you for sharing this Emily! I wish I had known of these options for my firstborn (an unplanned induction). It was horrible, long, painful & I believe still has impact on my child today. Fortunately, I learned more before my second child & was able to experience childbirth with a midwife. What a difference!! ❤️
LikeLike
Such an incredible story!! I now have things to “google”. Hopefully our newest edition to the family will be smooth.
LikeLike